The Internet Of Things Can Save 50,000 Lives A Year
It is the sixth leading cause of preventable death in the United States.[1] It kills more than 50,000 people every year in the U.S. alone and likely 10 times more worldwide, like crashing three jumbo jets every single day. It harms one in seven of those hospitalized under Medicare. It costs the U.S. government over $4 billion per year.[2]
Related Articles
- Know Your Regulations Before You Design Medical Electronics
- Know The FDA's New Guidelines For RF Wireless Medical Device Success
- Analog Signal Acquisition Enables Telemedicine
This problem frustrates caring doctors and nurses every day. The stories tear your heart out. Infants who will never see their homes. Schoolchildren lost to grieving parents. Grandparents whose wisdom will never again enlighten their families. Even worse, this problem has the unique capability to devastate those same caring professionals who have taken an oath to save lives.
What is this killer? Car accidents? Suicide? Guns? Drug abuse? No. Those problems all kill fewer people. The problem is preventable hospital error. Thousands and thousands of mistakes occur in hospitals every day. Catching them, or even tracking them, is frustratingly ad hoc. Soon, however, connectivity and intelligent distributed medical systems will dramatically reduce these errors. This is the revolution that the Internet of Things (IoT) promises for patient safety.
What’s Changed
This problem is not new. Thirty years ago, the last major change in healthcare system technology transformed hospital care through a simple realization: monitoring patients improves outcomes. That epiphany spawned the dozens of devices that populate every hospital room: pulse oximeters, multi-parameter monitors, ECG monitors, Holter monitors, and more.
Over the ensuing years, technology and intelligent algorithms improved many other medical devices, from infusion pumps for IV drug delivery to ventilators. Healthcare is much better today because of these advances. But errors persist.
Why? Today, these devices all operate independently. There’s no way to combine the information from multiple devices and intelligently understand patient status. Therefore, these devices issue many nuisance alarms. Fatigued healthcare staff members silence the alarms, misconfiguration goes unnoticed, dangerous conditions go unaddressed, and people die.
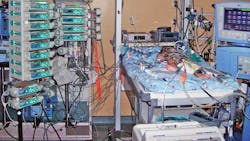
Consider the problem of interacting infusion pumps (Fig. 1). Often, multiple pumps will be used to deliver multiple drugs to a single patient. During heart surgery, for instance, drugs sedate the patient, stop the heart, start the heart, and more. Of course, there are many more devices too, including monitors and ventilators. A trained anesthesiologist orchestrates delivery and monitors status during surgery. The members of the team have their hands full coordinating all the signals to keep the patient safe.
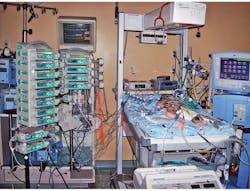
After surgery, the patient must transfer to the intensive care unit (ICU). This is a key risk moment. The drug delivery and monitor constellation must be copied from the operating room (OR) to the ICU. Today, the OR nurse calls the ICU on the phone and reads the prescription from a piece of paper. The ICU staff must then scramble to find and configure the correct equipment. The opportunity for small slips in transcription, coupled with the time criticality of the change, is fertile ground for deadly error.
Consider if instead these systems could work together in real time. The OR devices, working with a smart algorithm processor, could communicate the exact drug combinations to the electronic medical record (EMR). The ICU system would check this data against its configuration. Paper and manual configuration produce far too many errors. This connected system eliminates dozens of opportunities for mistakes.
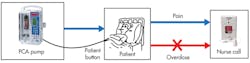
Once in post op, the danger is not over. Many patients use patient-controlled analgesia (PCA) systems. The PCA system allows the patient to self-administer doses of painkiller medication by pressing a button. The idea is that a patient with sufficient pain medication will not press the button and therefore will be safe from overdose.
PCA is efficient and successful. Millions of patients use it every year. Still, PCA overdose kills one to three patients every day in the U.S.[3] This seemingly simple system suffers from visitor interference, unexpected patient conditions, and (especially) false-alarm fatigue (Fig. 2).
Connectivity can also help here. For instance, low oximeter readings cause many alarms. They are only likely real problems if accompanied by a low respiratory rate. A smart alarm that checks both oxygen (SPO2) and carbon dioxide (CO2) levels would eliminate many distracting false alarms. An infusion pump that stopped administering drugs in this condition could save many lives.
Standards At Work
The list of procedures and treatments that suffer from unintended consequences is long. Today’s system of advanced devices that cannot work together is rife with opportunity for error. The common weakness: each device is independent. Readings from one device go unverified, causing far too many false alarms. Conditions easily detected by comparing multiple readings go unnoticed. Actions that can save lives require clinical staff interpretation and intervention.
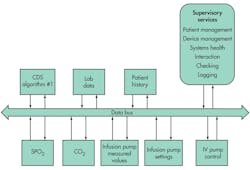
The leading effort to build such a connected system is the Integrated Clinical Environment (ICE) standard, ASTM F2761. ICE combines standards. It takes the data definitions and nomenclature from the IEEE 11073 (x73) standard for health informatics. ICE then specifies that data communications use the Data Distribution Service (DDS) standard. ICE defines control, data logging, and supervisory functionality to create a connected, intelligent substrate for smart clinical connected systems (Fig. 3).[4]
DDS is an IoT protocol from the Object Management Group (OMG).[5] While there are several IoT protocols, most focus on delivering device data to the cloud. DDS implements a data-bus architecture that understands and enforces correct interaction between participating devices. It focuses on the real-time data distribution and control problem. It also can integrate with the cloud or connect to other protocols to form a complete connected system. Its unique capabilities fit the medical device connectivity problem well.
For instance, while these examples are simple, networking medical devices in a clinical environment is quite challenging. Information flow mixes slow data updates with fast waveforms. Delivery timing control is critical. Integration with data from the EMR must provide patient parameters such as allergies and diagnoses. Appropriate monitor readings and treatment history must also be written to the EMR. Large hospitals must match data streams to patients, even as physical locations and network transports change during transfers between rooms. Devices from many different manufacturers must be coordinated.
ICE leverages DDS to address these clinical challenges. DDS models the complex array of variables as a simple “global data space,” easing device integration. Within the data space, the data-centric model elevates programs to exchange the data itself instead of primitive messages. It can sift through 1000 beds and 100,000 devices to find the right patient, despite moves. And, DDS is fast and operates in real time. It easily handles heart waveforms, image data, and time-critical emergency alerts.
Dr. Julian Goldman leads ICE. He is a practicing anesthesiologist with an appointment at Harvard Medical School as well as the director of bioengineering for the Partners hospital chain. His Medical Device Plug-n-Play (MDPnP) [6] project at the Center for Integration of Medicine and Innovative Technology (CIMIT)[7] connects dozens of medical devices together. MDPnP offers a free open-source reference platform for ICE. There are also commercial implementations, including one from a company called DocBox.[8] The CIMIT lab uses these implementations to prototype several realistic scenarios, including the PCA and OR-to-ICU transfer scenarios described here. It demonstrates what is possible with the IoT.
Hospital error today is a critical healthcare problem. Fortunately, the industry is on the verge of a completely new connected implementation. Smart, connected systems can analyze patient conditions from many different perspectives. They can aid intelligent clinical decisions in real time. These innovations will save lives.
This technology is only one benefit of the exciting future known as the Internet of Things. The IoT will connect many billions of devices together into intelligent systems. It will change every industry, every job, and every life. One of the first applications will extend those lives.
References
1. List of preventable causes of death, http://en.wikipedia.org/wiki/List_of_preventable_causes_of_death
2. Department of Health and Human Services, Office of Inspector General, Adverse Events in Hospitals, National Incidence in Medicare Beneficiaries, Nov. 2010 (QEI 06-09-00090)
3. Challenges to Implement A Standards Based ICE Platform, Tracy Rausch, Medical Device Interoperability Conference 2013.
4. ICE Standard: Integrated Clinical Environment, http://mdpnp.org/mdice.html
5. OMG Data Distribution Portal, http://portals.omg.org/dds/
6. Medical Device “Plug-and-Play” Interoperability Program, http://mdpnp.org
7. Center for Integration of Medicine and Innovative Technology, http://cimit.org/
8. DocBox, http://www.docboxinc.com
Stan Schneider is the CEO and founder of Real-Time Innovations (RTI). Previously, he was an independent technical and management consultant. He also managed one of the largest laboratories at Stanford University and developed networked communications systems at Sperry Computer Systems. He completed his PhD in electrical and computer science at Stanford University and holds a BS in applied mathematics and an MS in computer engineering from the University of Michigan.
[1] http://en.wikipedia.org/wiki/List_of_preventable_causes_of_death
[2] Department of Health and Human Services, Office of Inspector General. Adverse Events in Hospitals. National Incidence in Medicare Beneficiaries. Nov 2010. (QEI 06-09-00090)
[3] Challenges to Implement A Standards Based ICE Platform, Tracy Rausch, Medical Device Interoperability Conference 2013.
[4] http://mdpnp.org/mdice.html
[5] http://portals.omg.org/dds/
[6] http://mdpnp.org
[7] http://cimit.org/
[8] http://www.docboxinc.com
About the Author
Stan Schneider
CEO, Real-Time Innovations
Dr. Stan Schneider is CEO of Real-Time Innovations (RTI), the Industrial Internet of Things connectivity company. Stan serves as Vice Chair of the Industrial Internet Consortium (IIC) Steering Committee. He also serves on the advisory board for IoT Solutions World Congress, and chairs OpenFog's Fog World keynote committee. He was named Embedded Computing Design’s Top Embedded Innovator Award 2015 & IoTOne’s top-10 most influential in the IIoT 2017.He holds a PhD in EE/CS from Stanford.
Voice Your Opinion!
To join the conversation, and become an exclusive member of Electronic Design, create an account today!

Leaders relevant to this article: