This file type includes high-resolution graphics and schematics when applicable.
Over the next 15 years, global healthcare will transform due to a perfect storm of clinical imperative, financial burden, and increasingly informed and empowered patients. A growing population, steadily decreasing healthcare budgets, and the rise of chronic diseases are putting pressure on doctors, healthcare providers, and governments to look to technology to provide the solution to these challenges.
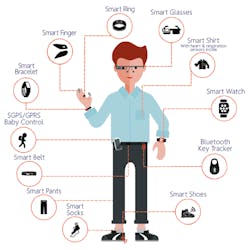
As a result, global healthcare and wellness is ideally placed to drive the adoption and maturity of the Internet of Things (IoT). The smart technologies commonly found on a person such as the smartphone, smartwatch, and new emerging technologies like smart plasters, will be at the heart of this revolution, providing insights that will deliver benefits to the physical, emotional, and mental self.
The smartphone is seen by many as their primary compute device—nearly two-thirds of American adults (64%) now own a smartphone according to survey done in 2015 by Pew Research. Today’s smartphone has fingerprint sensors, a camera, and the ability to connect via Bluetooth to activity monitors and medical devices like blood pressure monitors and ECG machines. Sensors are delivering ever more valuable and accurate data, and in the future we will see an increasing number of these distributed over the body cooperatively collecting and processing continuous data.
Moving forward, multiple sensors will be delivered within fabric garments, adhesive patches, and jewelry-type form factors, depending on personal choice and monitoring requirements. Together, this will transform the smartphone into an effective, personal vehicle for health management. Evidence of this can already be seen, with leading insurance providers in the U.S. subsidizing the cost of the Apple watch for their patients.
Impact on Healthcare, Personal Health, and the Market
Based primarily on face-to-face interactions between physician and patient (visit to the doctor, flu shot at work, or annual exam), existing protocols of treating patients are outdated and place undue pressure on current government and non-government structures. Remote health monitoring opens up a brand new protocol of how a physician treats a patient, with continuous information being collected from the patient—for example, someone coping with a chronic disease such as diabetes or congestive heart failure.
With this approach, physicians and loved ones are in a position to learn and provide better quality of care via deeper, more meaningful engagement with the patient. More actionable information is being continuously captured, ultimately reducing cost to the system. It will also result in curbing the growth of chronic diseases: Genomic research will rapidly spread to the clinical coalface, and this information must be enhanced with lifestyle monitoring to accurately predict the onset of chronic disease with enough warning to allow effective treatment.
The connected health market is expected to see something close to $117 billion revenue by 2020. As the smartphone and smartwatch evolve into the key vehicles for personal health, this will spurn massive innovations in wellness and medical sensors in, on, and off the body, and on the smartphone itself. New and emerging OEMs will be able to monetize the data collected versus just the hardware, enabling a vibrant ecosystem to develop. This stands in stark contrast to today’s model, which is limited to current major OEMs.
How Must Technology Evolve to Make This a Reality?
Three of the key areas we need to consider for the success of healthcare IoT can be broadly split into the categories of low-power medical and wearable devices; communication between sensors, smartphones (gateways) and the cloud; and security:
• For wearable and medical devices, battery life is imperative. ARM and many of our partners are looking into near-threshold voltage for embedded-class devices. The race is on to get to the lowest power with sufficient compute to obtain the maximum number of critical biometrics.
Key biometrics to be obtained include body fat; photoplethysmogram (PPG) for heart rate and respiration; electrocardiogram (ECG) to measure heart rate, rhythm, and general health of the heart; skin temperature; blood oxygen (SpO2); blood glucose; and blood pressure. Together, these form the crux of the core biometrics required to manage chronic diseases including, but not limited to, hypertension, diabetes, congestive heart failure, and COPD, as well as many of the patients who have comorbidities.
With a long history of ultra-low power and high performance, the ARM Cortex-M family of processors can run many of the algorithms involved in collecting these biometrics. Non-toxic batteries are also important to extend the usage of wearable devices over a long period of time.
• The smartphone is an ideal gateway platform for aggregating data from various medical sensors and for engaging with patients. It’s critical to have sufficient security and privacy in place to ensure that data is not stolen, and there’s sufficient ability to authenticate and validate the data from user and device.
As sensors on the body need to be able to last for multiple days without recharging, it’s imperative that the power budget used for communications is kept to the bare minimum while maintaining compatibility across billions of smartphones already deployed into the market. Already designed into billions of smartphones, Bluetooth Low Energy (BLE) is the most ubiquitous, low-cost radio solution for transmitting data from wearable sensors to be able to talk to the smartphone. ARM Cordio BLE solutions provide a platform for silicon vendors looking to design low-power silicon solutions for medical wearable applications to talk to the smartphone.
• Finally, in the cloud, beyond securing the data, we also need to act upon the data. Predictive analytics and machine learning can play a key role in reshaping the healthcare industry, starting with enabling device manufacturers, caregivers, and pharmaceutical players to improve the quality and the delivery of care we provide to the patient.
The ultra-low cost of BLE combined with low-power embedded processors such as the ARM Cortex-M family can enable developers to easily and cost-effectively integrate connectivity into billions of previously unconnected medical sensors and diagnostics tools. For example we will see connectivity being added to diagnostic devices ranging from HIV,glucose, pregnancy, and chem7, just to name a few.
It’s self-evident and imperative that data from such devices is kept secure, private, and only shared with trusted third parties with whom the patient consents to share this data. Solutions such as ARM CryptoCell and ARM TrustZone on both the sensors and the gateway are designed to ensure that data is kept absolutely secure and private from the time of acquiring that data (at the sensor) to the data validation, identity tagging, and consent acquisition of that data at the smartphone. As a result, that data can then be shared with trusted entities in the cloud whom the patient provides digital consent (for example, by swiping their fingerprint).
About the Author
Karthik Ranjan
Director of Healthcare and Emerging Technologies
Karthik Ranjan is the director of healthcare and emerging technology at ARM. Based in Seattle, Karthik is responsible for strategy in the healthcare vertical, helping the healthcare industry to utilize ARM’s low-power, high-efficiency technology in developing new services and increasing operational efficiencies. Prior to this, Karthik led ARM’s global carrier relationship team. Karthik has more than 16 years’ experience working in the consumer electronics industry with companies such as Intel, Microsoft, and Amino.
Voice Your Opinion!
To join the conversation, and become an exclusive member of Electronic Design, create an account today!

Leaders relevant to this article: